Beyond Hyperdensity: Identifying Rare Hypodense Artifacts in Dual-Energy X-ray Absorptiometry (DXA)
DXA imaging of the lumbar spine revealed a focal hypodense artifact over L1
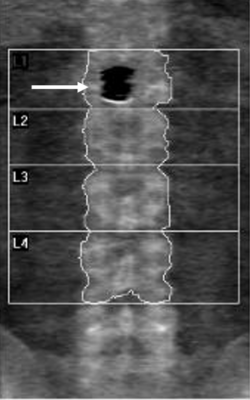
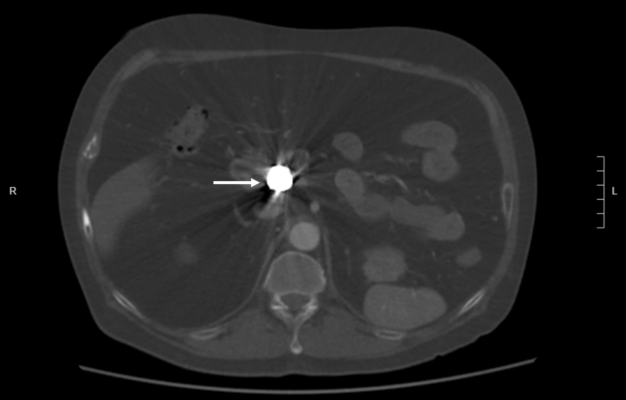
Recent CT imaging showed hypodense artefact over L1 on DXA image as a platinum-containing stent placed for a gastroduodenal artery aneurysm at L1 level
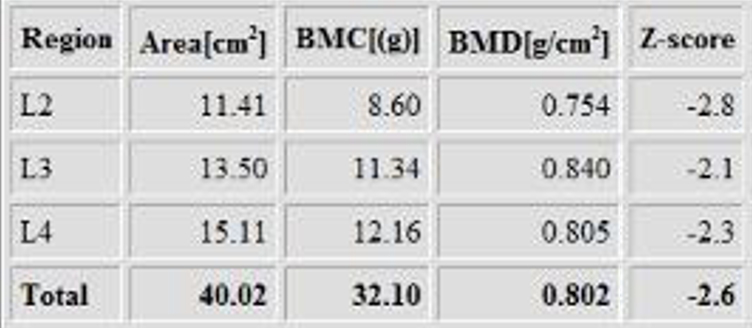
The Z-score with L1 excluded is -2.6
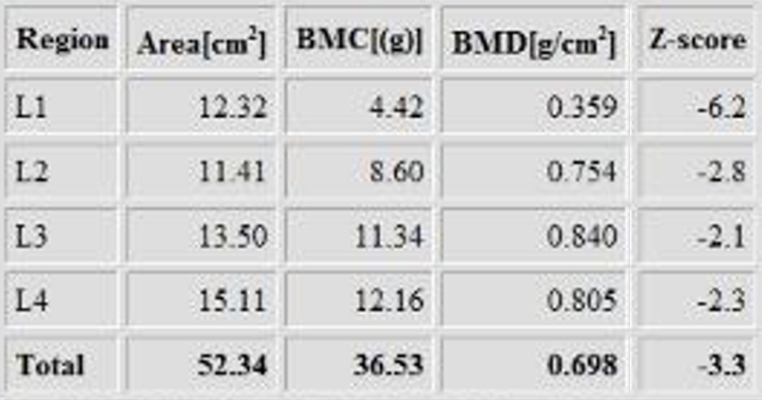
The Z-score with L1 included is -3.3
A hypodense region was noted in the left proximal femur on DXA image
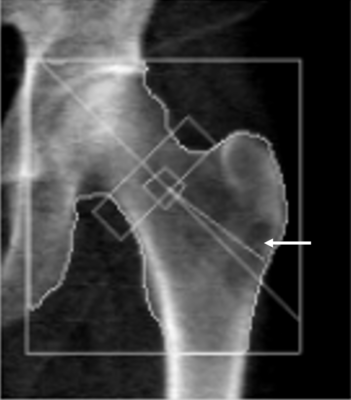
A known lytic bone metastasis with cortical disruption seen on CT
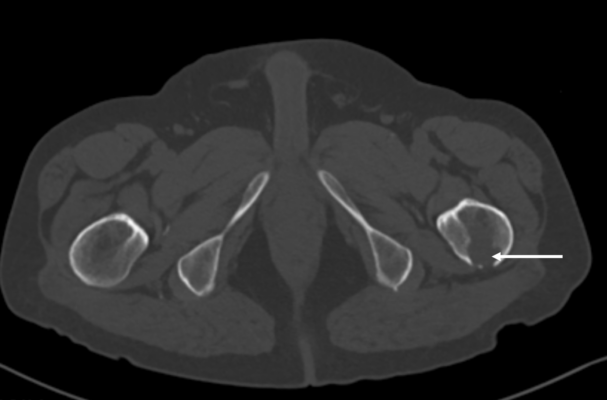
For those patients with hypodense artifact identified in the hip, consider scanning the other hip or the forearm

Dual-energy X-ray absorptiometry (DXA) is the gold standard for measuring bone mineral density (BMD). While most exogenous materials (e.g., calcification, standard surgical hardware) present as hyperdense artifacts that falsely elevate BMD, certain high-density materials and lytic pathologies can manifest as “hypodense” artifacts (the “black hole” effect), leading to diagnostic challenges. A 47-year-old male with metastatic renal cell carcinoma (mRCC) on the tyrosine kinase inhibitor axitinib was referred for DXA following multiple atraumatic rib fractures. DXA imaging of the lumbar spine revealed a focal hypodense artifact over L1 (Fig 1A). Recent CT imaging for correlation identified this as a platinum-containing stent placed for a gastroduodenal artery aneurysm (Fig 1B). Consequently, L1 was excluded from the Z-score calculation to prevent inaccurate assessment. Additionally, a hypodense region was noted in the left proximal femur (Fig 2A), which matched a known lytic bone metastasis with cortical disruption previously seen on CT (Fig 2B). This case illustrates that high-atomic-number metals—such as platinum, tantalum, or lead—can paradoxicaly cause “black holes” on DXA because their extreme attenuation exceeds the software’s threshold for bone, causing it to incorrectly subtract the area as background or soft tissue. In this patient, the clinical picture was further complicated by lytic metastases from mRCC, which also produce focal hypodensity. Clinicians must maintain a high index of suspicion when encountering hypodense artifacts on DXA. Accurate interpretation requires correlation with anatomical imaging (such as radiographs, CT) and clinical history. Known causes of hypodense artifacts include lytic bone lesions, laminectomy sites, high-density metals (platinum, tantalum), and spina bifida.
Wong Wai Chung, Nuclear Medicine Unit, Queen Elizabeth Hospital, Hong Kong
Morgan, S. L., Lopez-Ben, R., Nunnally, N., Burroughs, L., Fineberg, N., Tubbs, R. S., & Yester, M. V. (2008). “Black hole artifacts”—a new potential pitfall for DXA accuracy?. Journal of Clinical Densitometry, 11(2), 266-275.
Albano, D., Agnollitto, P. M., Petrini, M., Biacca, A., Ulivieri, F. M., Sconfienza, L. M., & Messina, C. (2021). Operator-related errors and pitfalls in dual energy X-ray absorptiometry: how to recognize and avoid them. Academic Radiology, 28(9), 1272-1286.